Just as the COVID-19 pandemic began to wane, new surges in cases and hospitalizations have popped up in several states. While a portion of these spikes can be attributed to more testing, the increase in hospitalizations is evidence of a more problematic trend. In an effort to halt the surge, states like Florida that had reopened quickly are now reclosing restaurants and gyms, not the route they expected to take. The point is that the virus is likely to be with us for at least months, if not years, to come. We must not let our guards down, especially for populations at risk. One of those includes people living with a substance use disorder (SUD).
Suspected opioid overdoses rose 18% in March, 29% in April, and 42% in May.[1]
Social isolation is hard on most people, but for those living with SUD, it can be deadly. Being around peers and family help patients feel connected and supported—both essential for a successful recovery. But with COVID-19, in-person AA meetings and other support groups have been cancelled or have moved online. While a virtual meeting is better than no meeting at all, it lacks the intimacy of an in-person group and makes communication among the group more challenging. This can lead to depression and anxiety, which can fuel relapse.
Counselors and therapists, too, have moved from in-person appointments to telehealth. Again, while this approach is better than no appointment, it, too, comes with many challenges. Patients who live within close quarters to others may find it difficult to find privacy during a video call, which means they may not be fully forthcoming with the counselor for fear of being overheard. Telehealth also removes the ability to drug test or screen patients for signs of abuse prior to an appointment.
When SUD patients lose a job due to businesses shuttering, they lose an important social network as well as financial independence, both of which can lead to relapse.
Another factor that has led to increasing opioid deaths during COVID is the interruption in the drug supply chain, which has led many dealers to use synthetic and potentially lethal substances as a replacement.[2] For patients who’ve been through detox, taking the same dose they were previously accustomed to—whether “pure” or not—the result is more likely to be overdose and death.
Removing the Isolation Barrier
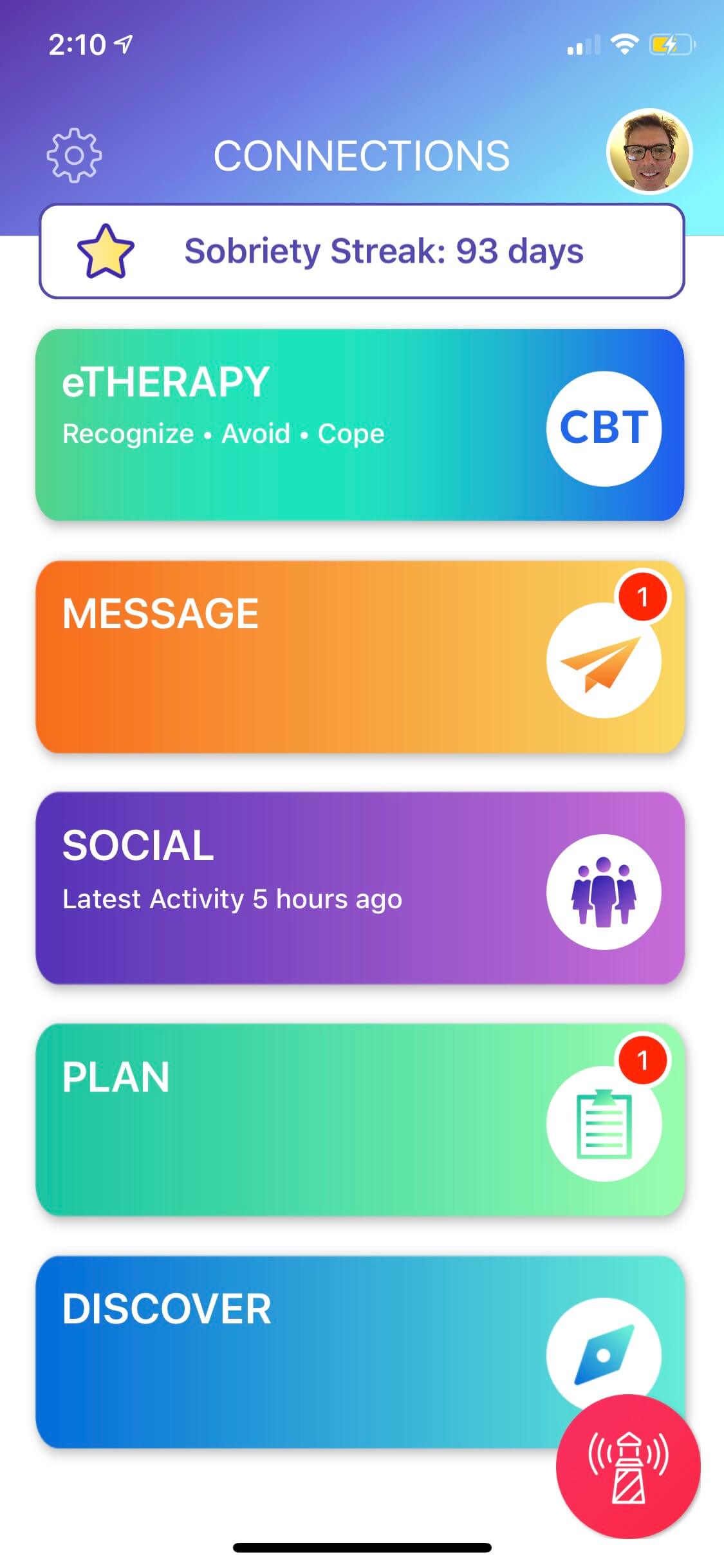
The best way to mitigate all of these risks is through digital technology that keeps patients connected with their peers, clinicians, and families in a way that is safe and always available. The Connections App from CHESS Health can do just that by giving patients the tools they need right in the palm of their hands through a smartphone app.

The Connections App is part of an integrated care platform that provides multiple support features, including: anonymous group messaging with peers, sobriety tracking, daily surveys, recovery tracking, educational and motivational content, and crisis line access. Connections also includes a companion app that helps clinicians engage with patients, while tracking and analyzing their progress. Having this tool helps clinicians provide more informed, personal, and effective support to their patients.
“It’s very important for us to stay connected. Thank goodness for this app to help us with that.” “It’s cool to talk to people that are going thru the same thing as me at different levels of recovery.”– Patient Feedback on Connections App
Much research has been conducted on the use of digital tools for SUD treatment. Patients who use these tools are more likely to keep appointments, adhere to care plans, attend more treatment days, and they are more motivated to stick with their programs.[3] Research on the Connections App also shows a lower likelihood of relapse.[4]
There’s No Time to Wait
The latest statistics are proof of the devastation this pandemic is having on those living with SUD. Unfortunately, relief efforts have failed to adequately address this issue. Of the $2.5 trillion in relief funds, only $425 million has been allocated for mental health and SUD treatment. As the Washington Post points out, this is “barely more than a hundredth of one percent.”[5] In other words, SUD providers and organizations are going to have to look for innovative ways to help patients make it through this difficult time. And it’s critical that we act soon as some healthcare experts are warning that COVID-19, or some version of it, may be with us for years.[6]
We’ve already gotten a small glimpse of the challenges we face as we try to reopen the economy in the face of this pandemic. It is, unfortunately, a learn-as-we-go scenario. But that’s not the case when it comes to treating patients with SUD. We know the dangers they’re facing and we have proven technology to help reduce the impact of isolation. The situation at hand is dire and we must do all we can now to keep the scourge of overdose from becoming the next pandemic.
[1] https://www.washingtonpost.com/health/2020/07/01/coronavirus-drug-overdose/
[2] ibid.
[3] https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3419880/
[4] Published studies available at www.chess.health/evidence
[5] https://www.washingtonpost.com/health/2020/07/01/coronavirus-drug-overdose/
[6] https://science.sciencemag.org/content/368/6493/860.full
